
PCOS statistics: What the numbers really mean
PCOS is common, yet there’s a lot we don’t know about this condition due to gaps in the data and a lack of funding for PCOS research. Yet while the PCOS statistics can’t tell us everything, they illustrate how far we’ve come in understanding this disease.
Polycystic ovarian syndrome (PCOS) may be one of the most common endocrine disorders, but it’s far from the most studied health conditions. Like many hormonal health problems, PCOS is often underdiagnosed, suffers from a lack of research funding, and often takes over four years to go from first symptoms to diagnosis.
PCOS statistics like these can inform our understanding of this condition. To help you find them without spending hours upon hours researching, we compiled an up-to-date, comprehensive look at PCOS prevalence, common symptoms, health risks, and more.
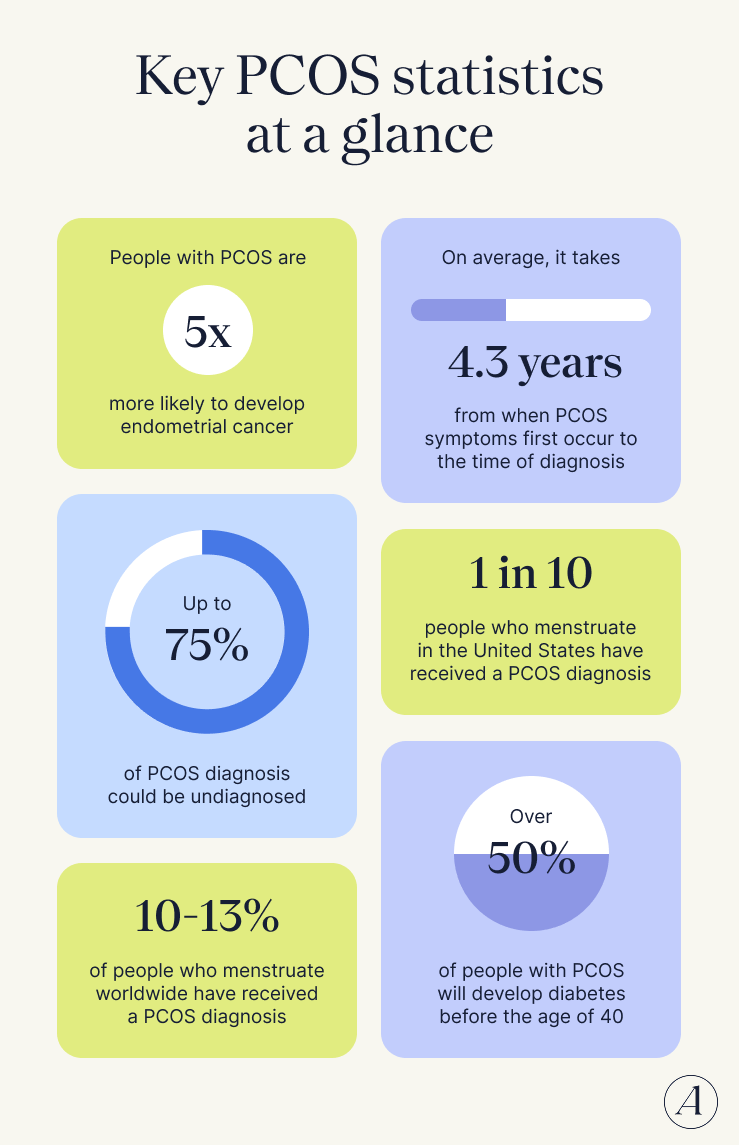
Key PCOS statistics at a glance
- 10-13% of people who menstruate worldwide have received a PCOS diagnosis, according to the World Health Organization. WHO notes that PCOS is commonly underdiagnosed, so the actual prevalence may be even higher.
- One in ten people who menstruate in the United States have received a PCOS diagnosis, according to the U.S. Office on Women’s Health. The office notes that this refers to one in ten individuals who are of childbearing age, which they define as 15 to 44.
- Up to 75% of PCOS diagnosis could be undiagnosed, according to a 2023 peer-reviewed paper in Diagnostics. “We can only estimate the prevalence based on who is formally diagnosed and assume from there,” says Maribelle Faucett, WHNP, women’s health nurse practitioner and clinical manager at Allara Health, “This creates a major gap in understanding the true extent and impact of PCOS beyond what we already know because of underdiagnosis.”
- Over 50% of people with PCOS will develop diabetes before the age of 40, according to the Centers for Disease Control and Prevention. PCOS doesn’t exist in a vacuum; it’s associated with or increases the risk for many conditions, including insulin resistance and diabetes.
- On average, it takes 4.3 years from when PCOS symptoms first occur to the time of diagnosis, according to a 2023 peer-reviewed article in BMC Women’s Health. It’s important to remember this is an average, meaning some people—especially those with inadequate access to healthcare—may wait even longer.
- People with PCOS are up five times more likely to develop endometrial cancer, according to a 2023 meta-analysis in Oncology Letters. “I strongly emphasize the importance of preventing endometrial hyperplasia, what happens before endometrial cancer, to all of my patients,” says Faucett, “There can be a disconnect in understanding the risks associated with having only one to three periods per year.”
PCOS prevalence: How common is PCOS?
Determining PCOS prevalence is hard because the condition is underdiagnosed and PCOS stats vary quite about a bit depending on the population they’re extracted from. Data may vary by country, ethnicity, lifestyle, and more. Here’s a brief recap of what current research suggests about this condition’s prevalence.
PCOS prevalence worldwide
According to the World Health Organization, 10-13% of people who menstruate have PCOS. By contrast, a 2026 meta-analysis in Critical Public Health places PCOS prevalence worldwide somewhere between 5-20%. Additionally, PCOS is on the rise: In 1990, it affected 36.7 million people globally while in 2021, 69.5 million people had PCOS. It’s unclear, however, whether this is due to an actual increase in the syndrome or an increase in diagnoses due to greater awareness and improved diagnostics.
A 2025 meta-analysis found the following PCOS rates by continent:
- Europe: Up to 6.27%
- Americas: Up to 6.33%
- Asia: Up to 11.15%
The prevalence of PCOS in Africa could not be determined due to a lack of high quality studies on the continent. This highlights another important gap in medical research.
PCOS prevalence in the United States
The CDC states that PCOS may affect up to five million people in the United States. Similarly, the U.S. Office on Women’s Health conservatively estimates it impacts one in ten people who menstruate.
To date, there has only been one study completed on prevalence by US region (and none by state). That study placed regional rates at:
- 47.5% of people with PCOS live in the South
- 23% live in what the North Central region (aka the Midwest)
- 10.3% live in the Northeast
- 18.7% live in the West
PCOS prevalence in other countries
There are a lot of gaps in PCOS prevalence in other countries as well. We do have some nationwide stats, such as these examples:
- India: As high as 11.33%
- Pakistan: As high as 52% in some Pakistani populations
- Phillipines: Exact number unknown, but the Philippines has the highest rate of PCOS-related infertility in the Asia-Pacific region
- UK: About 10%, according to the UK’s National Health Service (NHS)
- Australia: Around 12% of people who menstruate between the ages of 16 and 29
- Spain: 28.3% in people who menstruate and are overweight or obese and 5.5% of individuals who are lean
- Mexico: 6.6%, though there are limited studies from this country
- Japan: 5-8% of people who menstruate
- China: 6-10%, with prevalence increasing 65% in the last decade

PCOS underdiagnosis: How many people go undiagnosed?
One in ten people who menstruate having PCOS is already a big deal. What’s even more staggering is how many people may have this condition but are not currently diagnosed:
- Up to 75% of PCOS cases are estimated to undiagnosed
- On average, it takes 4.3 years between when PCOS symptoms start to time of diagnosis
- Research into PCOS is also underfunded. While PCOS has a similar prevalence and impact as rheumatoid arthritis (RA), PCOS received $31.84 million in government funding from 2016 to 2022 while RA research received $262.40 million in that same timeframe.
Faucett explains that one of the main reasons PCOS is underdiagnosed is that some symptoms may be attributed to another condition by mistake. If someone with PCOS has acne, for example, a dermatologist may only treat the acne and not refer them to a PCOS specialist.
“Everyone presents differently,” Faucett explains, “And for providers who don't see PCOS often, I often see uncertainty in making the diagnosis based on existing (and changing) criteria.”
PCOS demographics: Who has PCOS?
When looking at PCOS facts, we also need to take into account the condition’s demographics, or how common the condition is across different races, ethnicities, and age groups.
PCOS by race and ethnicity
PCOS can affect anyone who menstruates, though it’s more common in people of South Asian, African, or Middle Eastern descent. The exact stats vary, but a 2022 study on the ethnicities of 244,642 adolescents diagnosed with PCOS in a Northern California hospital system offers an idea of what the breakdown may look like in the US:
- 4.2% of Asian or Pacific Island adolescent
- 2.9% of Hispanic/Latinx adolescents
- 2.4% of non-Hispanic white adolescents
- 2.1% of Black adolescents
Another study compared the ethnicities of women referred by a primary care provider to a specialist. It found that 84% of the referral group was non-Hispanic white women, while 53% of those who sought specialist help without a referral were African American. This highlights how access to specialists may not be equal for everyone and the importance of being a self-advocate when it’s unfortunately necessary.
PCOS by age
PCOS can occur anytime after someone reaches puberty. That said, it’s most likely to be diagnosed when someone is in their 20s or 30s. It is possible that people experience symptoms for years before they get diagnosed, and unfortunately we don’t have a ton of data on the age of onset.
An age-related stat we do have is that symptoms often subside after 35, with people over that age reporting more regular menstrual levels and lower levels of androgen (male) hormones.
How common are different PCOS symptoms?
PCOS symptoms vary widely. They can include symptoms associated with the menstrual cycle, changes to hair growth and skin health, and fatigue. Not everyone will experience every symptom and even a single symptom, such as painful periods, can feel slightly different for everyone.
That said, the most common symptoms are:
- Heavy periods: Up to 70% of people with PCOS report heavy periods during their menstrual cycle.
- Period pain: Dysmenorrhea is the medical term for painful or crampy menstruation. PCOS dysmenorrhea prevalence is quite significant, with 30% of people with PCOS reporting painful periods.
- Irregular periods: Almost 70% of people with PCOS experience oligo-anovulation, which is when eggs aren’t released as often from the ovaries. This leads to irregular periods and may increase the change of infertility.
- Severe acne: 12-14% of people with PCOS commonly report clinical acne as one of their symptoms.
- Excess hair on face and body: Hirsutism, excessive body and facial hair growth on people who menstruate, can occur for many reasons, though there’s a higher prevalence of hirsutism in populations with PCOS. 72% of hirsutism cases are found in those with PCOS.
- Hair loss on scalp: Androgenic alopecia, the medical term for hair loss on the scalp, is a symptom for somewhere between 5-50% of people with PCOS. This range is so big due to lack of research.
- Sleep disturbances: 60.5% of people with PCOS reported mild sleep disturbances in one study. 29.7% had chronic sleep disturbances. Disturbances may include reduced sleep quality or duration, fragmented sleep, daytime sleepiness, and difficulty staying asleep.
- Fatigue: People with PCOS are more likely to report fatigue or low energy than those without.
How does PCOS affect fertility and pregnancy?
While it is possible to start a family with this condition, some studies suggest 70-80% of people with PCOS struggle with fertility. In an Australian study, for example, people with PCOS were four times as likely to report difficulty getting pregnant.
People with PCOS also have a marginally high chance of miscarriages (15% compared to 14.8% for those without this condition in one study). In addition, contrary to the usual expectation that miscarriage rates will decrease the further someone is into their pregnancy, patients with PCOS show a slightly increased risk of later-term miscarriage than those without the condition.
Struggling doesn’t mean that family growth is impossible. In a study from the Netherlands, 1,779 people with PCOS underwent fertility treatments. Within the first year, 37% were pregnant and eventually had a healthy birth.
What conditions are associated with PCOS?
As if PCOS wasn’t enough on its own, it also increases the risk or is associated with a few other medical conditions, including:
- Anxiety: 42% of people with PCOS have anxiety compared to 8.5% without it.
- Depression: People with PCOS are 2.5 times more likely to experience depression compared to those without this condition.
- Insulin resistance: The prevalence of insulin resistance in PCOS is quite high. It impacts as many as 95% of people with PCOS who have obesity and 75% of people with PCOS who don’t have obesity.
- Metabolic syndrome: About 43% of adults with PCOS and as much as one third of adolescents with PCOS have metabolic syndrome, a cluster of health problems that increase the risk for type 2 diabetes and heart disease.
- Diabetes: Insulin resistance can progress to type 2 diabetes. In fact, over 50% of people with PCOS will develop type 2 diabetes before they turn 50.
- Heart disease: PCOS significantly increases the risk for cardiovascular diseases, especially if it’s present alongside other conditions like metabolic syndrome or type 2 diabetes.
- Endometrial cancer: Those with PCOS are at a higher risk for endometrial cancer. The American Cancer Society says people with PCOS have a two to three times higher risk. Other meta-analyses suggest the chance of getting endometrial cancer is as much as five times higher.
- Vitamin D deficiency: Some small scale studies suggest a higher Vitamin D deficiency prevalence in populations with PCOS. This vitamin supports the immune system, healthy bones, and may play a small role in fertility.
- Sleep apnea: In one meta-analysis, 35% of people with PCOS also had sleep apnea, a chronic condition where breathing starts and stops when sleeping.
- Fatty liver disease: The presence of fatty liver disease is somewhere between 10-32% for people with PCOS, compared to 0.7-4.2% in people without this condition.
What these numbers mean — and what they don’t capture
These PCOS statistics highlight how many people are affected by the condition and the varied effects it can have on someone’s life and health. They remind us that PCOS looks different for everyone and that many people are underrepresented in PCOS research.
When asked what the stats don’t show, Faucett reflected, “They don’t show much courage it takes for patients to seek good care after being dismissed so many times, and the challenging journey it can be to feel better.”
Key takeaways
- PCOS prevalence may vary since it’s underdiagnosed, but it’s commonly cited as impacting around one in ten people who menstruate.
- PCOS greatly affects overall quality of life. It has a wide range of possible symptoms and an association with many other health conditions, such as metabolic syndrome and type 2 diabetes.
- Getting a diagnosis often takes a while, and there are real barriers to receiving specialist care for many people.
- But it’s not all bad news; many researchers, clinicians, and healthcare organizations, such as Allara Health, are committed to getting rid of those barriers and expanding access to PCOS speciality care. Hopefully in five years time, the stats reflect greater access to care and more research for this condition.
Frequently asked questions (FAQs)
Why is PCOS so common now?
PCOS is a hormonal condition that’s becoming increasingly common. While researchers don’t know the exact reason why, it could be because more cases are being diagnosed than before, increasing the official numbers. Other factors, such as an increase in the consumption of ultra-processed foods and people living a more sedentary life, may also contribute.
At what age does PCOS usually start?
Most people with PCOS receive the diagnosis in their 20s or 30s. However, PCOS can start at any age after puberty.
What percent of people with PCOS have fertility issues?
PCOS infertility statistics can range quite a bit, though some studies suggest that up to 70-80% of people with PCOS have fertility issues. This doesn’t mean that everyone with fertility issues won’t be able to start a family, just that they may benefit from fertility treatment if they wish to do so.












