
How to lose weight with PCOS: A science-backed, sustainable guide
Losing weight with PCOS often feels like an uphill battle, because the condition comes with hormonal imbalances that can make weight management tricky. But tricky does not equal impossible. Ahead, we’ll dive into how to lose weight with PCOS in a sustainable, effective way.
If you have PCOS and it feels impossible to lose weight, even when you do everything right, you’re not imagining it. Researchers from Australia tracked weight gain in people with PCOS and those without for 19 years. Even when the study participants’ lifestyles were the same, people with PCOS experienced greater weight gain than those without.
The good news is that the same study suggests that changes to diet, physical activity levels, and other lifestyle factors led to significant weight loss in people with PCOS. That means an empowering, sustainable PCOS weight loss plan has a pretty good chance of creating meaningful change. Plus, it may also improve more important markers of health, like energy levels, PCOS symptom severity, and overall quality of life.
Continue reading to learn how to lose weight with PCOS, no crash diets or hunger pangs required. And it goes without saying, but this guide is for those who want to lose weight, which does not have to be the goal of every person with PCOS.
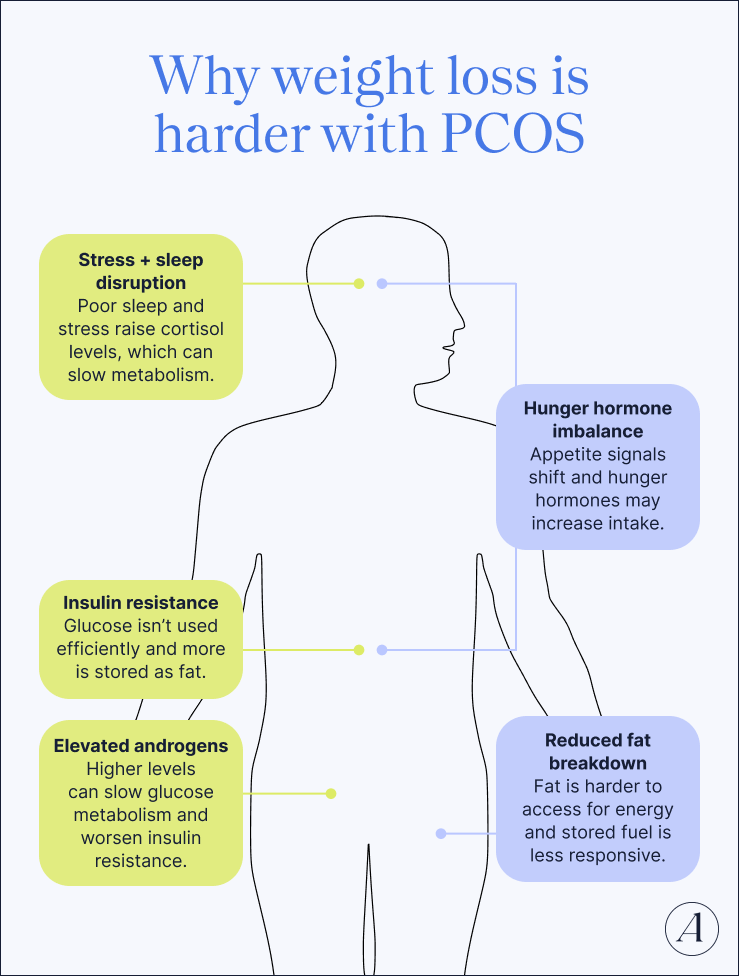
Why is it harder to lose weight with PCOS?
The main reason it’s harder to lose weight with PCOS is the condition’s predisposition to insulin resistance. Insulin is a hormone involved in blood sugar regulation and fat storage.
“As you consume food, it gets broken down to carbohydrates and then, essentially, glucose,” explains Tiffany Pham, D.O., a board-certified OB/GYN at Allara Health, “This glucose is in your bloodstream, and in order to get from your bloodstream into the cells and tissue that utilize glucose for energy, it needs a bridge. That bridge is insulin.”
If the bridge is wobbly (aka the body becomes less responsive to insulin), it’s referred to as insulin resistance. Insulin resistance can increase fat storage in two main ways:
- More unused glucose to store: When insulin resistance occurs, there’s more unused blood sugar, which the body stores as fat.
- Excess fat release: When insulin resistance occurs, insulin is less effective at its many responsibilities, which include regulating lipolysis, the process by which your body breaks down fats. That lack of regulation means a higher amount of fat is released into the bloodstream before it can be used for energy, which then contributes to insulin resistance further, creating a vicious cycle and more fat storage.
Additional PCOS factors that impact weight management
While an increased risk for insulin resistance is the main reason PCOS makes it harder to lose weight, other factors work against weight management too:
- Higher androgen levels: With PCOS, you typically have higher androgen levels,” says Dr. Pham, “that actually can disrupt the process of glucose metabolism as well.” Glucose metabolism is the process of breaking down food into glucose and then getting it to cells and tissue that can use it, which insulin plays a role in too. When this process is disrupted, the body stores more fat.
- Increased cortisol levels: PCOS is associated with higher levels of normal cortisol production. While cortisol is nicknamed the stress hormone, it also impacts metabolism, often leading to greater fat storage, particularly around the belly.
- Imbalanced hunger hormones: People with PCOS may have higher levels of ghrelin and lower levels of leptin. The two hormones play opposing roles—ghrelin increases appetite and food cravings, while leptin suppresses appetite. That means PCOS may lead to increased hunger cues.
- Uneven fat-to-muscle ratio: PCOS increases the risk of obesity and metabolic syndrome. These two conditions make it more difficult to lose weight. Felice Ramallo, MSCN, RDN, LD/CDN, lead dietitian at Allara, explains that both these conditions create an imbalance of fat to muscle. “When fat to muscle is out of balance,” she says, “fat tissue releases more inflammatory molecules that get us stuck in a self-perpetuating cycle of weight gain and inflammation.”
Does everyone with PCOS struggle with weight?
Weight gain is common but not inevitable with PCOS. Somewhere between 40-60% of people with PCOS are overweight or obese, meaning the other half or so of people fall into the category of “lean PCOS.”
In people with lean PCOS, leptin levels are in a more typical range, meaning appetite cues aren’t higher than they should be, and insulin resistance is less likely to occur. With this type of PCOS, weight loss is probably not the right focus. In fact, losing too much weight can lead to low energy levels, a higher chance of depression and osteoporosis, and feeling lightheaded or dizzy. It can also exacerbate PCOS’ menstrual cycle irregularity and may contribute to infertility.
A healthcare provider can help you determine if you fall within the overweight, normal, or underweight weight range. For a rough estimate, you can use the CDC’s BMI calculator, noting that it is a guideline, not a substitute for guidance from a PCOS specialist.
Can losing weight improve PCOS symptoms?
Weight loss for PCOS isn’t just about the number on the scale; the lifestyle changes someone develops along the way are the most important part. Developing healthier habits can reduce PCOS symptom frequency and/or severity with (or without) weight loss.
How to lose weight with PCOS
“Oftentimes people with PCOS feel like they’re fighting an uphill battle because of the underlying root cause of PCOS and insulin resistance,” says Dr. Pham, “but that doesn't mean weight loss is impossible. It definitely makes it harder, but nowadays we have a lot of different tools to help.”
Instead of looking for one cure or solution, people with PCOS should instead build a toolbox of healthy habits and weight management strategies, such as the ones below.
Nutrition that supports blood sugar and hormones
Eating a healthy diet can support weight loss, and we’re using the vague term “healthy diet” on purpose. The best diet for pcos weight loss is individualized, meaning it can look different from person to person.
That said, there are a few general guidelines that might help, but there’s a lot of room for customization based on what you like to eat, any food allergies or dietary restrictions, and how much time you have to cook.
There are also some small changes that can help improve insulin sensitivity:
- Mix and match food types: “Pair carbs with protein sources (like animal proteins, tofu, beans) and fiber (leafy greens, cruciferous vegetables, berries, nuts, seeds),” recommends Ramallo. She recommends eating at least 25 to 30 grams of fiber per day and at least 1.2g/kg protein daily.
- Protein and fiber come first: To blunt blood sugar response, eat the fiber and protein on your plate before any non-fiber carbs.
- Don’t forget the dressing: “Dressing veggies with vinegar-based dressings changes the pH in the digestive tract enough to also slow down the absorption of carbs,” says Ramallo.
Focus on portion sizes
When planning your meals, it’s also important to be like Goldilocks—prep portions that aren’t too little or too big, but instead just right for your activity level, age, and gender. The U.S. Department of Agriculture has a free tool that can provide portion recommendations based on these factors.
You may also want to “front load” caloric consumption. Eating more earlier in the day works with insulin sensitivity, not against. “We better utilize glucose and have smoother blood sugar curves when eating the same meal earlier than later,” explains Ramallo, “Having a solid breakfast and lunch, with a lighter dinner can work with our body's rhythms for blood sugar management.”

Exercise that works with PCOS
There’s a lot to love about exercise. It enhances insulin sensitivity, lowers stress levels, and may either help burn calories (if cardio-based) or build muscle that burns calories more when resting (if strength-based).
The American Society for Reproductive Medicine’s PCOS guidelines highlight two recommended physical activity levels depending on someone’s goals:
As for the best exercise type, that depends on your personal preferences and current activity levels. Dr. Pham mentions that patients often ask her for specific workouts to try, and she counters with a few questions of her own:
- What do you do currently? Going from zero to HIIT or CrossFit four times a week isn’t a realistic (or healthy) exercise goal. Tailor your exercise goal so it meets you where you are.
- What type of movement can you do consistently? Going on daily walks, for example, will lead to better results than one extreme sprint workout a month.
- What type of movement do you enjoy? If you hate running or yoga, don’t do it. Workouts you enjoy are easier to show up for than ones you dread.
Nonexercise activity time and PCOS
Official workouts aren’t the only time we move our bodies (at least in an ideal world). A sedentary lifestyle is associated with a worse overall quality of life, increased insulin resistance, and trouble losing weight. That means you not only want to complete official workouts but pay attention to your non-exercise activity time (NEAT) as well.
As someone who spends most of my workday seated at my computer, I get that increasing NEAT is hard. Luckily, there are small ways to increase your NEAT time, even if you work a desk job:
- Choose the stairs over the elevator when possible
- Take a short walk after meals (bonus points since walking after eating improves insulin sensitivity)
- Park further out when shopping so you have to walk further to the store
- Set a timer to take stretching breaks when seated for long periods
- Engage in active hobbies, like gardening or pottery making
You can also track your daily step count, which is a great way to add a quantitative challenge to your NEAT goal. Ramallo often recommends aiming for 7,500 steps a day, progressing to 10,000 a day if it works for your lifestyle.
Sleep and stress matter more than you think
Two hidden factors for PCOS and weight loss are sleep and stress. “People often underplay the importance of sleep and chronic stress,” says Dr. Pham, “They can actually make things like insulin resistance even worse for patients, and sleep and chronic stress also have roles in appetite regulation.”
For sleep, aim for seven to nine hours a night, ideally waking up and going to sleep around the same time each day, even on weekends. People with PCOS are more likely to struggle with sleep apnea, so treating that condition (or any others that make it difficult to fall and stay asleep) can help.
Stress management can help regulate cortisol levels and reduce emotional eating. It may also regulate appetite-related hormones like ghrelin and leptin.
Ways to reduce stress include:
- At-home stress management techniques: Consider mindfulness practices, meditation, breathwork, journaling, or other ways to reduce stress. Like with exercise, the technique you enjoy the most, not the one you feel you “should” do, is the one you’ll probably engage in most consistently.
- Therapy: Counseling, especially cognitive behavioral therapy, is an essential tool for anyone who finds it difficult to manage stress on their own.
- Behavioral programs related to diet: Some people with PCOS find programs on food-related emotions and behaviors reduce stress and provide extra accountability during their weight loss journey.
Supplements and medications for weight support in PCOS
If lifestyle changes alone aren’t enough, medication for PCOS weight loss can help. Medications like metformin and GLP-1s can help reduce insulin resistance, which may indirectly contribute to weight loss.
Some GLP-1s, such as Wegovy, are also FDA-approved for weight loss. Clinical trials suggest GLP-1s lead to weight loss and improved insulin sensitivity in people with PCOS, though it’s important to note that medications are in addition to a healthy lifestyle, not in place of it.
“We have to remember that weight loss medications are not magic bullets,” explains Dr. Pham, “You still have to have the foundation of lifestyle, nutrition, and movement, regardless of what medication you're on, to see the benefits.” The same goes for supplements, which have a very modest effect on weight compared to GLP-1s and other weight loss drugs.
A healthcare provider, ideally one specializing in hormonal health like the experts at Allara, can recommend the best medications for you, as well as any supplements for specific nutrient gaps in your diet.
When weight loss feels impossible
“When you have a condition like PCOS, the playing field is not level,” says Dr. Pham, “It's like asking someone to run an obstacle course with one hand tied behind their back.” No one wants to run an obstacle course with one hand, just like doing all the things to lose weight without seeing progress isn’t fun either.
“If after time, there is still no progress, it's definitely time to work with a registered dietitian and medical provider, like the teams at Allara,” says Ramallo. A qualified healthcare team can order any medical tests to get a more comprehensive view of your situation, evaluate your PCOS symptoms, and recommend any medications, supplements, nutrition strategies, or lifestyle changes that can help in your specific situation.
“If you need the extra help, don't be ashamed of it,” says Dr. Pham, “There's such a stigma around weight management medications, and just weight management in general, that people don't realize that most of us are already trying to do the foundational things, yet we don’t always see the results.” Sometimes, an extra tool like a prescription for a weight loss drug or a meal plan created by a registered dietitian who regularly works with people with PCOS makes all the difference.

A note on diet culture, shame, and PCOS
When it comes to PCOS and weight gain, the last thing you want to feel is shame or as if the number on the scale is in any way a reflection of your worth. Spoiler alert: It’s not.
If you feel that pursuing weight loss is right for your health journey, go for it (in a sustainable way that doesn’t sacrifice your peace of mind). If instead you want to focus on boosting your energy levels, relieving PCOS symptoms, or regulating your cycle, those are all great goals too.
For those who are seeking to lose weight, remember that there’s no set plan to follow. You (and your healthcare team) can tailor weight loss strategies to what “enough” looks like to you.
“Focus on getting your ‘enoughs,’” advises Ramallo, “Enough nutrition, physical activity, sleep, and stress management. Fill your cup with the things you need, and allow your body to get everything it needs to grow into a healthier you.”
The bottom line
- PCOS can make weight harder but not impossible. With a customized plan in place and a hormonal healthcare team behind you, maintaining a healthy weight with PCOS is possible. Plus, many of the lifestyle strategies and medications in that plan may help with other PCOS symptoms, such as fatigue or acne.
- Some of the most effective weight loss strategies for people with PCOS include eating a well-balanced diet, exercising consistently, increasing non-exercise activity time, managing stress, getting enough sleep, and using any medications a healthcare provider prescribes, such as Metformin or GLP-1s.
- Not everyone with PCOS needs to lose weight. If you’re wondering if you do, consult a hormonal healthcare provider, such as the team at Allara, who can assess where you’re at currently and create an empowering plan to achieve your health goals.
Frequently asked questions (FAQs)
What is the fastest way to lose weight with PCOS?
The best way to lose weight with PCOS is by implementing healthy habits you can stick with, supported by medication when recommended by a healthcare provider. For many people with this condition, lifestyle changes include eating more whole foods, getting regular movement, serving themselves healthy portion sizes, practicing stress management techniques, and getting seven to nine hours of sleep a night.
Why is it hard to lose weight with PCOS?
It’s hard to lose weight with PCOS for a few reasons. The first is that PCOS increases the risk of insulin resistance. When insulin doesn’t work as intended, it can lead to excess glucose that the body stores as fat. PCOS also impacts ghrelin and leptin, two hormones involved and appetite regulation, resulting in more hunger cues and cravings. Last but not least, there is an association between PCOS and higher normal cortisol levels; increased cortisol can promote more fat storage, especially around the belly.
Can weight loss cure PCOS?
There is no cure for PCOS. Weight loss may reduce symptoms and help with insulin resistance, though it’s not always required. If someone is happy with their current weight, there is no need to lose extra pounds. Instead, they can focus on lifestyle changes and treatment that more directly impact PCOS and insulin sensitivity, such as walking after meals, aiming to eat more whole foods than processed foods, and practicing stress management strategies, like breathwork or journaling.












